
SensVita
Radio-Based Cardiopulmonary monitoring device.
Simplifying Cardiopulmonary Monitoring
At SensVita, I contributed to the development and early production of a non‑contact, radio‑based cardiopulmonary monitoring system built into a bedpad for use in hospitals and retirement homes. The system provides continuous, unobtrusive measurement of heart rate and respiration without electrodes or wearables, expanding access to longitudinal physiological data. The final iteration will incorporate automated analysis that tracks long‑term trends.
My role spanned the full development pipeline - from validating the sensing modality and building the initial signal‑processing pipeline, to designing the physical enclosure and establishing a scalable production workflow for the bed‑pad assembly used in pilot deployments.
I am currently developing the industrial design and manufacturing plan to streamline production and support future commercialization.
Highlights:
Tracks Heart & Respiratory Metrics
Contactless Sensing
Machine Learning Compatibility
Partners: SensVita
Role: Software & Hardware Engineer, Production Lead
Timeline: Sept 2025 - Present
The Challenge
I validated the sensing modality by collecting my own biometric data by lying down directly on top of the sensor, and then building a basic signal‑processing pipeline to isolate cardiac and respiratory components.
To assess performance across sleep positions, I recorded data in multiple orientations. Signal quality depended primarily on distance: positions with the heart closest to the sensor (lying on stomach) produced clearer cardiac signals, while lying on the side or back improved respiratory signal fidelity.
I validated accuracy by running a parallel ECG and benchmarking my algorithm’s heart-rate estimates against it, achieving 96% agreement.
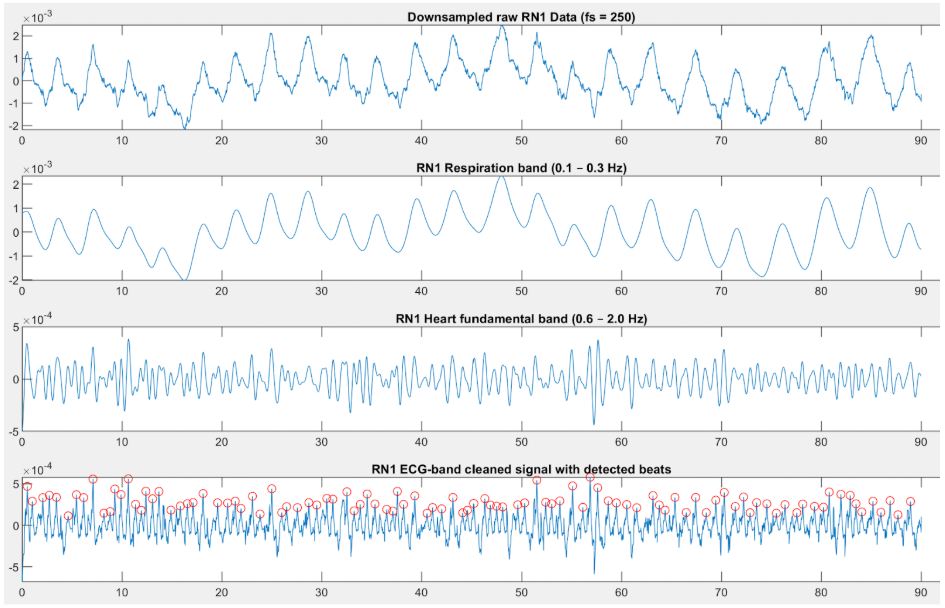
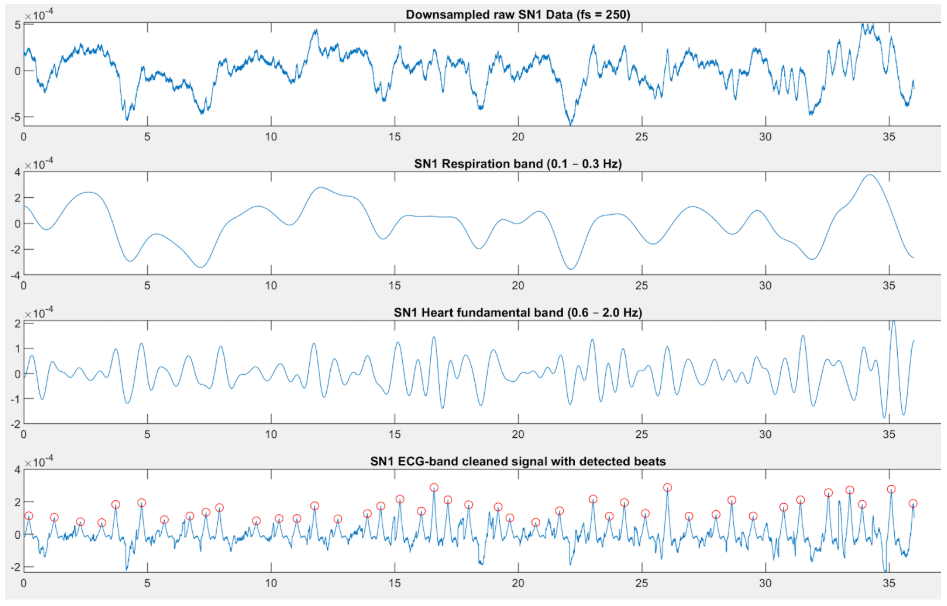
Respiratory signal drives the main waveform. Image 1 was collected lying on the right side, resulting in a clear respiratory waveform. Image 2 was collected lying on the stomach, compressing the lungs, creating an irregular respiratory waveform, but a clearer cardiac waveform.
I then led the mechanical design of the sensor enclosure, selecting materials to balance durability, comfort, and electrostatic neutrality. Early prototypes were hand‑built from sewn EVA foam, enabling rapid iteration on thickness, stiffness, and fit. This design used two EVA foam sheets with corner cutouts to cleanly route the four antenna interfaces. Future iterations will integrate a custom PCB bonded directly to the antenna ports, embedding the radio to reduce bulk, simplify assembly, and improve robustness.
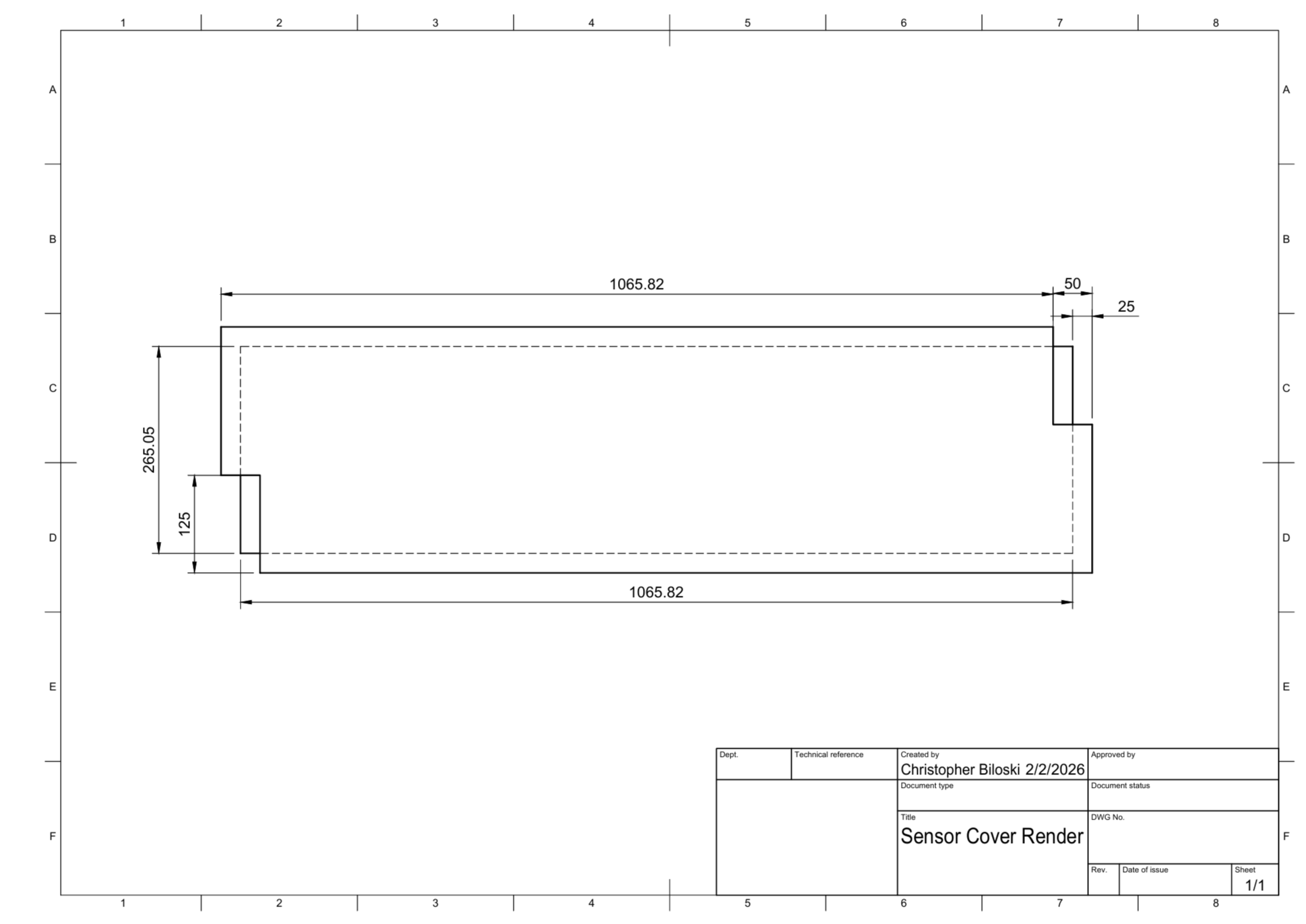
Pre-production case specifications.
Next, I spearheaded the transition from prototype to production for the bed‑pad assembly, evaluating 90 soft‑goods manufacturers and categorizing them by capabilities, scale, and material expertise to find partners suited for medical‑grade fabrication. I selected Herculite for their healthcare‑fabric specialization and, through their network, partnered with NY Orthopedics for manufacturing. I supplied CAD files, material specs, and assembly requirements, resulting in our first professionally produced, production‑ready case and a repeatable workflow for pilot and early deployments.

CAD render of the case-antennae assembly.
With production established, I am now leading the industrial design, refining the prototype into a user-ready product. In parallel, I am developing a scalable manufacturing plan - refining materials, assembly methods, and cost structure to support efficient production and future commercialization.

CAD render of the current pad design.